Clearest Health — Recover Your Out-of-Network Revenue
Rate this Tool
Average Score
Total Votes
Select your score (1-10):
Detail Information
What
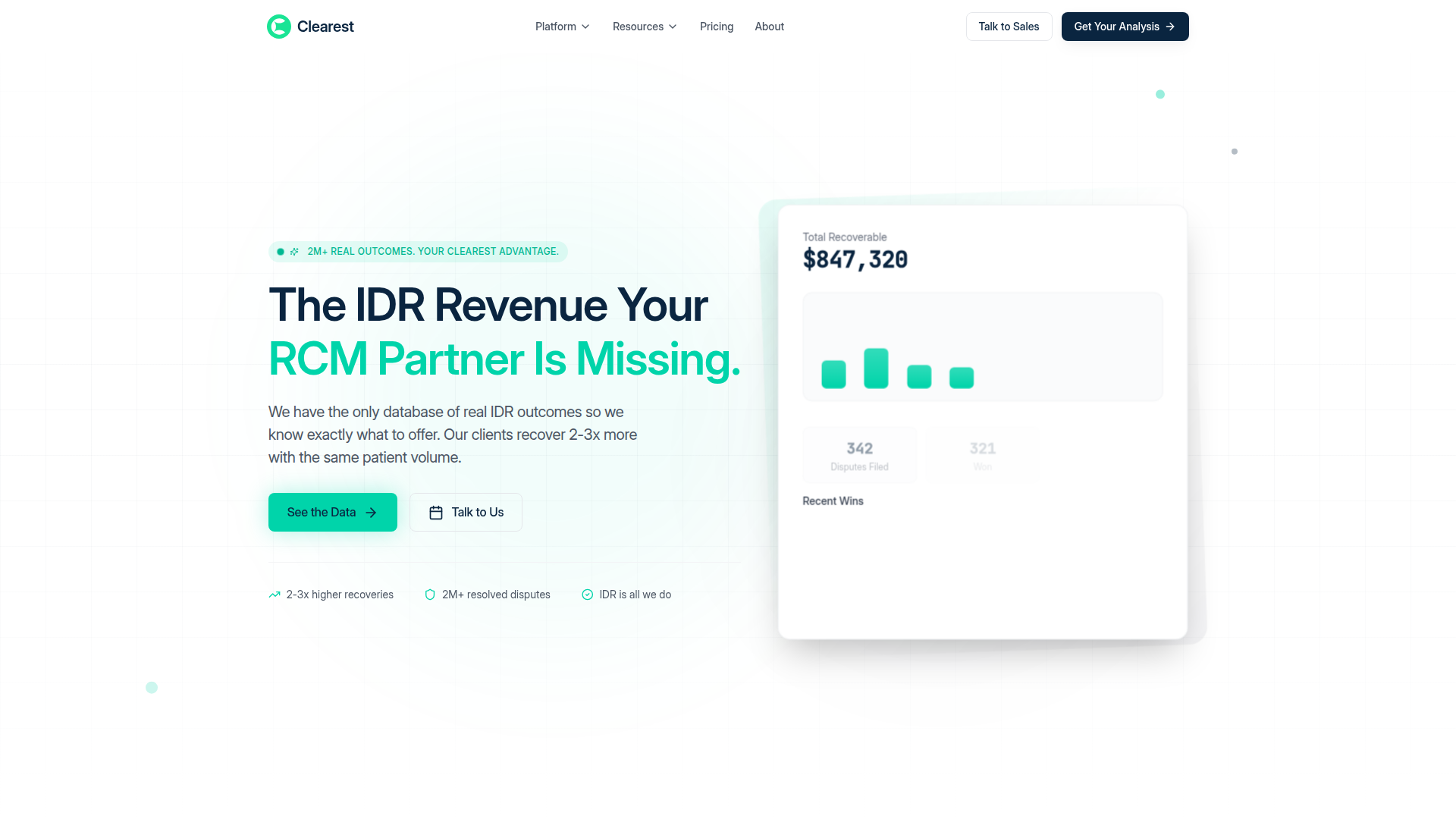
Clearest Health is a specialized revenue recovery platform and service focused on independent healthcare practices with out-of-network claims that may qualify for Independent Dispute Resolution (IDR) under the No Surprises Act. Its core value proposition is using a proprietary database of resolved IDR outcomes to help providers determine stronger offer amounts and recover more from underpaid claims.
The workflow described on the page is straightforward: Clearest analyzes claims, identifies worthwhile IDR opportunities, files disputes using evidence from comparable resolved cases, and manages the process end to end. The product appears positioned as a focused complement or alternative to a general revenue cycle management partner, specifically for practices that already file disputes or should be filing them but lack reliable pricing intelligence.
Features
- IDR opportunity analysis: Reviews underpaid claims and identifies disputes worth pursuing, helping practices focus effort on claims with higher expected recovery value.
- Proprietary pricing database: Uses matched IDR outcomes by CPT code, payer, region, and facility type to support more informed dispute pricing than billed charges or estimates.
- Evidence-ready dispute documentation: Builds dispute packets with comparable payment data so arbitrators receive supporting evidence rather than unsupported offer amounts.
- Offer optimization: Recommends pricing levels based on historical dispute outcomes, which can improve recovery potential without relying on guesswork.
- Payer-specific strategy: Applies payer intelligence on settlement behavior and thresholds, which may help tailor filing tactics by insurer rather than using a uniform approach.
- End-to-end case management: Handles filing, documentation, and status tracking through the dispute process, reducing administrative load for provider organizations.
Helpful Tips
- Validate data coverage for your specialty: For IDR tools, benchmark quality depends on how well the product covers your procedure mix, payer mix, geography, and facility type.
- Compare against your current RCM workflow: If an existing partner already manages denials and disputes, assess where IDR-specific pricing intelligence would materially improve outcomes rather than duplicate work.
- Review the evidence model carefully: In this category, the practical differentiator is often whether comparable-payment documentation is specific and credible enough to influence arbitrators.
- Ask for a claim-level recovery methodology: Forecasts are more useful when they show how opportunities are ranked, how offer amounts are derived, and which claims are likely not worth filing.
- Separate confirmed claims from marketing comparisons: The page makes strong performance claims; buyers should confirm definitions, time-to-resolution assumptions, and whether results vary by payer and procedure type.
OpenClaw Skills
Clearest Health could likely fit into OpenClaw as a healthcare revenue intelligence workflow centered on out-of-network underpayments and IDR case preparation. A useful OpenClaw skill could ingest EOBs, remittance files, and claim exports, flag likely underpaid claims, classify them by CPT, payer, and region, and route the right cases into a dispute preparation queue. If Clearest exposes structured outputs or reports, another likely workflow could summarize recovery opportunities for practice leaders and revenue cycle teams.
A broader OpenClaw agent layer could likely turn Clearest-based insights into operational automation for ambulatory groups, surgical practices, and specialty clinics. Examples include a claims triage agent, an arbitrator-evidence drafting assistant, a payer-pattern monitoring workflow, or a revenue forecasting dashboard that estimates likely IDR recovery by specialty and payer. These are inferred use cases rather than confirmed native integrations, but the combination could meaningfully shift healthcare finance teams from reactive underpayment follow-up to more data-led dispute strategy.
Embed Code
Share this AI tool on your website or blog by copying and pasting the code below. The embedded widget will automatically update with the latest information.
<iframe src="https://www.aimyflow.com/ai/clearesthealth-com/embed" width="100%" height="400" frameborder="0"></iframe>
Explore Similar Tools
Valerie Health
Valerie Health is an AI healthcare operations platform that helps independent provider groups modernize front-office workflows such as referral management, scheduling, fax and document handling, and patient engagement. For clinical operations leaders and healthcare executives, it can use AI to reduce administrative burden, improve workflow consistency, and give teams clearer visibility into patient access and growth operations.
Healthcare | Claude by Anthropic
Claude is a HIPAA-ready AI tool for healthcare organizations that helps health systems and startups handle prior authorizations, claims appeals, patient message triage, and clinical documentation with more accuracy, safety, and compliance. For clinicians, operations teams, and healthcare developers, it can reduce administrative workload and speed review, scribing, and routing tasks so more time goes to patient care and higher-value decisions.
Amazon Connect Health - AWS
Amazon Connect Health is an AWS healthcare AI platform for providers and health technology developers that helps with patient verification, appointment management, patient insights, ambient clinical documentation, and medical coding within existing care workflows. In AI-enabled healthcare operations, it can help clinicians, contact center teams, and coders spend less time on documentation and scheduling while keeping human review and source traceability in place.
Zinng
Zinng is an AI answering service that handles 24/7 and after-hours calls, identifies emergencies, sends SMS alerts, and can support appointment scheduling for practices and other businesses, especially dental and healthcare offices. For front-desk teams, practice managers, and office owners, it can reduce missed urgent calls and streamline follow-up with transcripts and scheduling workflows.
AI Clinical Documentation for Therapists | AutoNotes
AutoNotes is AI-powered clinical documentation software that helps therapists and behavioral health professionals generate compliant progress notes, SOAP and DAP notes, treatment plans, and session summaries from written, dictated, uploaded, or recorded sessions. For therapists, social workers, and practice teams, it can reduce administrative documentation work while preserving editable, structured records and continuity across sessions.
AI Form Filler - Fill out PDF forms with Instafill.ai
Instafill.ai is an AI form-filling tool that extracts fields from PDF and Word documents, autofills them from multiple data sources, and helps teams in document-heavy sectors like healthcare, legal, insurance, government, real estate, and finance complete paperwork faster. In AI-driven operations, it can reduce manual re-entry and review time for administrative, compliance, and case-processing roles while preserving visibility into how each field was filled.
#1 Healthcare Automation Platform - Keragon
Keragon is a HIPAA-compliant healthcare automation platform that helps healthcare companies connect 300+ integrations and automate workflows without code. For healthcare operations and IT teams, this can reduce manual process work and support faster, more reliable coordination across systems in AI-driven healthcare environments.
HIPAA Compliant AI Tools for Healthcare | HIPAA Compliant Claude
Hathr.ai is a HIPAA-compliant AI tool for healthcare that helps professionals summarize information, analyze large documents, generate letters, and automate clinical and administrative workflows while keeping sensitive data private in AWS GovCloud. For healthcare teams and related compliance-heavy roles, it can speed documentation, record review, and research while reducing privacy risk in AI-assisted work.